Why Internal Quality Audits Are Essential for Hospital Accreditation Readiness
Hospital accreditation is no longer a “nice-to-have” badge of honor — it has become a fundamental requirement for healthcare organizations committed to safe, reliable, and high-quality care. Whether your hospital is preparing for NABH, JCI, or another national or international accreditation, one truth remains unchanged:
Internal quality audits (IQAs) are the foundation of true accreditation readiness.
Yet many hospitals still underestimate them. They rush to update documentation just weeks before an external assessment, pressure staff to memorize SOPs, and scramble to fix long-standing gaps under intense time pressure. The result? Stress, repeated assessments, financial losses, and in some cases, failed accreditation.
This blog aims to shift that mindset.
If your organization is pursuing accreditation, understanding and implementing strong internal quality audits is the single most effective strategy you can adopt.
In this article, you will learn:
- Why internal audits are essential — not optional
- What areas they must cover
- How they elevate safety and clinical quality
- How they directly strengthen NABH/JCI readiness
- Common mistakes hospitals make
- Best practices for designing high-performing audit systems
- Real-world examples of how internal audits accelerate accreditation
By the end, you will have a clear, practical roadmap to dramatically enhance your hospital’s accreditation journey.
- What Are Internal Quality Audits?
Internal quality audits are structured, systematic evaluations that assess whether a hospital’s clinical, administrative, and operational processes meet defined standards. These may include:
- National standards (NABH, NQAS, CGHS)
- International frameworks (JCI, ACHS, ISO 9001)
- Internal SOPs
- Statutory and regulatory requirements
Put simply:
An internal audit is your hospital’s own health check — a way to verify whether systems, staff, and processes are functioning as expected.
Unlike external audits conducted by accredited assessors, internal audits are performed by trained internal teams. Their key objectives are to:
- Identify compliance deviations
- Detect risks before they become issues
- Strengthen process standardization
- Improve quality indicators
- Prepare the hospital for external assessments
Internal audits are proactive — not reactive. They help hospitals find and correct problems long before an assessor arrives.
- Why Internal Audits Are the Backbone of Accreditation Readiness
Accreditation programs focus heavily on patient safety, quality improvement, governance, and risk reduction. But accreditation is not earned on the assessment day — it is earned through continuous readiness, built over months of disciplined internal auditing.
Here’s why internal audits are indispensable.
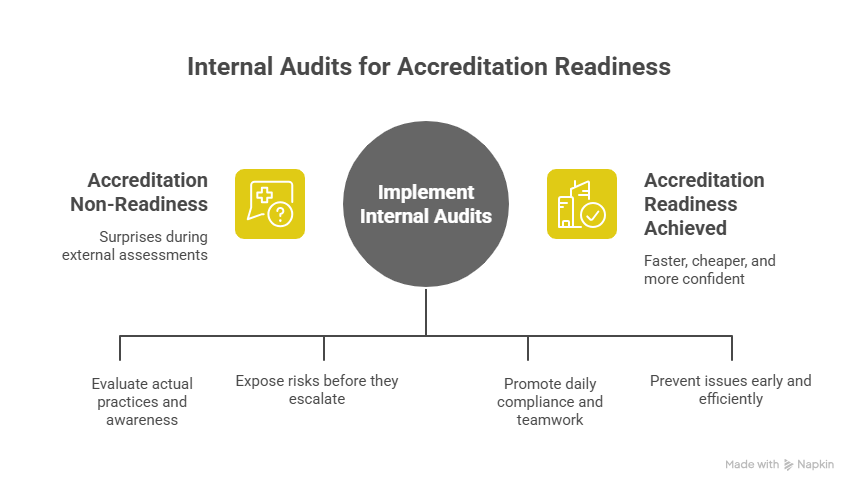
- They Provide a Realistic Readiness Check
Many hospitals mistakenly assume that having updated documents is enough. But assessors evaluate:
- Actual practices
- Staff awareness
- Patient safety behaviors
- Evidence of improvement
- Traceability of care processes
- Response to incidents and deviations
Internal audits reveal the true state of readiness by identifying whether:
- Staff actually follow SOPs
- Documentation matches day-to-day operations
- Compliance is consistent across departments
- Evidence is complete, current, and retrievable
Common findings during internal audits include:
- Inconsistent hand hygiene practices
- Poor medication storage or missing temperature logs
- Blocked fire exits
- Incomplete OT sterilization/biomedical logs
- Missing consent form signatures
- Incomplete medical records
- Expired calibration certificates
If external assessors identify these issues, hospitals may face major nonconformities, repeat assessments, financial penalties, and heightened safety risks.
Internal audits eliminate these surprises.
- They Strengthen Patient Safety and Clinical Quality
Patient safety is at the heart of every modern accreditation standard.
Strong internal audits expose risks long before they escalate into incidents. Audits often uncover:
- Medication errors
- Infection control breaches
- Incomplete clinical documentation
- Unsafe patient transfers
- Gaps in emergency preparedness
- Near misses that staff may hesitate to report
Research consistently shows that hospitals with structured internal audit programs achieve better patient outcomes.
By identifying and addressing these gaps proactively, hospitals create a safer, more predictable environment for patients and staff.
- They Build a Culture of Continuous Improvement
Accreditation is not an event — it is a continuous journey.
Internal audits reinforce this mindset by:
- Promoting daily compliance
- Reducing last-minute panic
- Encouraging teamwork and accountability
- Making quality everyone’s responsibility
- Creating learning opportunities
- Embedding a “do it right every day” culture
When internal audits are integrated into routine operations, compliance becomes natural rather than forced.
- They Reduce Accreditation Costs and Delays
Accreditation can be resource-intensive. A lack of readiness often leads to:
- Consultant re-engagement
- Repeat assessments
- Additional training needs
- Delayed accreditation
- Staff frustration
- Reputation risk
A strong internal audit program prevents these issues early.
Hospitals that invest in continuous auditing typically achieve accreditation:
- Faster
- With fewer nonconformities
- With more confident staff
- With significantly lower overall cost
III. Key Areas Internal Audits Must Cover to Meet Accreditation Standards
Accreditation standards take a holistic view of hospital operations. Internal audits must do the same.
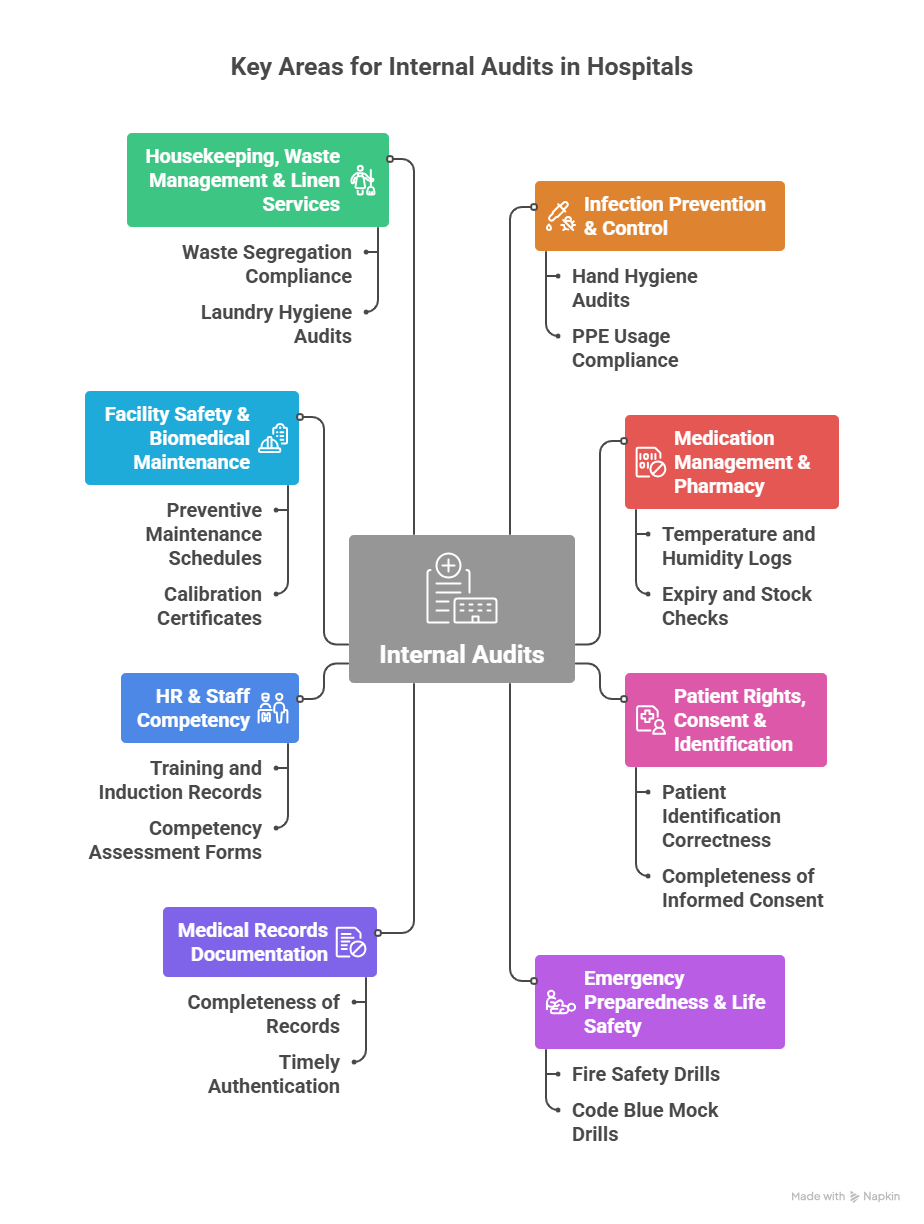
Below are the core areas every hospital must evaluate.
- Infection Prevention & Control (IPC)
- Hand hygiene audits
- PPE usage compliance
- Biomedical waste segregation
- Sterilization and autoclave validation
- OT/CSSD sterility checks
- Isolation room compliance
- Needle stick injury reporting
IPC remains one of the most heavily scrutinized areas during accreditation.
- Medication Management & Pharmacy
- Temperature and humidity logs
- Expiry and stock checks
- Controlled drug register
- Labelling and storage practices
- High-alert medication protocols
- Prescription completeness audits
- Ward-level medication storage compliance
Medication errors are a major risk during assessments.
- Patient Rights, Consent & Identification
- Patient identification correctness
- Completeness of informed consent
- Communication of patient rights
- Protection of vulnerable groups
- Privacy and confidentiality measures
These audits ensure legal, ethical, and safe patient care.
- Emergency Preparedness & Life Safety
- Fire safety drills
- Code blue and disaster mock drills
- Functional fire extinguishers
- Accessible evacuation routes
- Crash cart readiness
- Staff awareness interviews
Preparedness is a critical component of both NABH and JCI.
- Medical Records Documentation
- Completeness and legibility of records
- Proper patient assessments
- Timely authentication
- Consistent handovers
- Electronic record audit trails
Documentation lapses remain among the most common nonconformities.
- HR & Staff Competency
- Training and induction records
- Competency assessment forms
- Credentialing and privileging
- Appraisal records
- Department-wise staff awareness
Assessors will speak directly to staff — internal audits prepare them.
- Facility Safety & Biomedical Maintenance
- Preventive maintenance schedules
- Calibration certificates
- Hazard identification checklists
- Biomedical equipment logbooks
- Adequate safety signage
A safe physical environment is a core accreditation requirement.
- Housekeeping, Waste Management & Linen Services
- Waste segregation compliance
- Laundry hygiene audits
- Housekeeping checklists
- Pest control records
- Chemical storage compliance
These areas directly impact IPC performance.
- Quality Indicators, Audit Trails & Incident Reporting
- Monitoring of KPIs (infection rates, medication errors, etc.)
- RCA documentation
- CAPA effectiveness
- Incident reporting culture
Accreditation bodies look closely at evidence of improvement — not just records.
- How Internal Audits Prepare Hospitals for NABH/JCI Assessments
Internal audits build the foundation needed to meet the four pillars of accreditation:
- Documentation
- Implementation
- Evaluation
- Continuous improvement
Here’s how they support readiness.
- Mapping Nonconformities to Standards
Robust internal audits map each finding to the specific NABH/JCI standard and chapter.
This helps hospitals:
- Focus on high-risk areas
- Prioritize improvements
- Plan resources
- Track standard-wise compliance
This structure reduces guesswork and eliminates surprises during assessment.
- Running Mock Assessments
Mock audits replicate the external assessment experience, including:
- Document review
- Tracer methodology (for JCI)
- Staff interviews
- Patient interviews
- Process observations
- Safety evaluations
- Emergency drill simulations
Mock audits drastically improve staff confidence and familiarity with assessment expectations.
- Implementing Corrective & Preventive Actions (CAPA)
Audits add value only when findings are acted upon.
Effective CAPA includes:
- Root cause analysis
- Corrective action planning
- Responsibility assignment
- Timeline definition
- Documented closure
- Effectiveness verification
Strong CAPA systems lead to sustained compliance and meaningful improvement.
- Tracking Progress Through Dashboards
Dashboards allow hospitals to track:
- Compliance trends
- Open vs. closed findings
- Training completion
- Incident patterns
- High-risk areas
- Department-wise performance
These visuals give leadership the data they need to make timely, strategic decisions.
- Real-World Examples of Internal Audits Driving Accreditation Success
Example 1: 250-Bed Hospital Preparing for NABH
Challenges included:
- Fire safety compliance
- IPC inconsistencies
- OT sterile supply workflows
The hospital implemented:
- Monthly IPC audits
- Quarterly fire drills
- Weekly biomedical and pharmacy audits
- Dashboard-based CAPA tracking
Result:
Achieved NABH accreditation in 14 months with minor observations.Example 2: Multispecialty Hospital Targeting JCI
Challenges:
- Patient communication
- Tracer methodology
- Medication management
Interventions:
- Multidisciplinary internal audits
- Strengthened documentation
- Enhanced emergency preparedness
- Staff training
Result:
Achieved JCI accreditation with zero major nonconformities.- Common Mistakes Hospitals Make During Internal Audits
Understanding typical pitfalls can help avoid costly setbacks.
- Treating Audits as a Checklist Activity
Superficial audits lead to repeated issues.
Solution:
Train auditors and focus on observation-based evaluations.- Conducting Audits Too Close to Accreditation
Last-minute audits leave no time for correction.
Solution:
Audit throughout the year to maintain continuous readiness.- Not Involving Frontline Staff
Frontline gaps are often the root cause of noncompliances.
Solution:
Interview staff and observe real-time practices.- Poor CAPA Follow-Up
Findings without closure have no value.
Solution:
Use dashboards and enforce leadership review.- Untrained Auditors
Without training, serious gaps may remain hidden.
Solution:
Develop trained, multidisciplinary audit teams.VII. Best Practices to Strengthen Internal Quality Audits
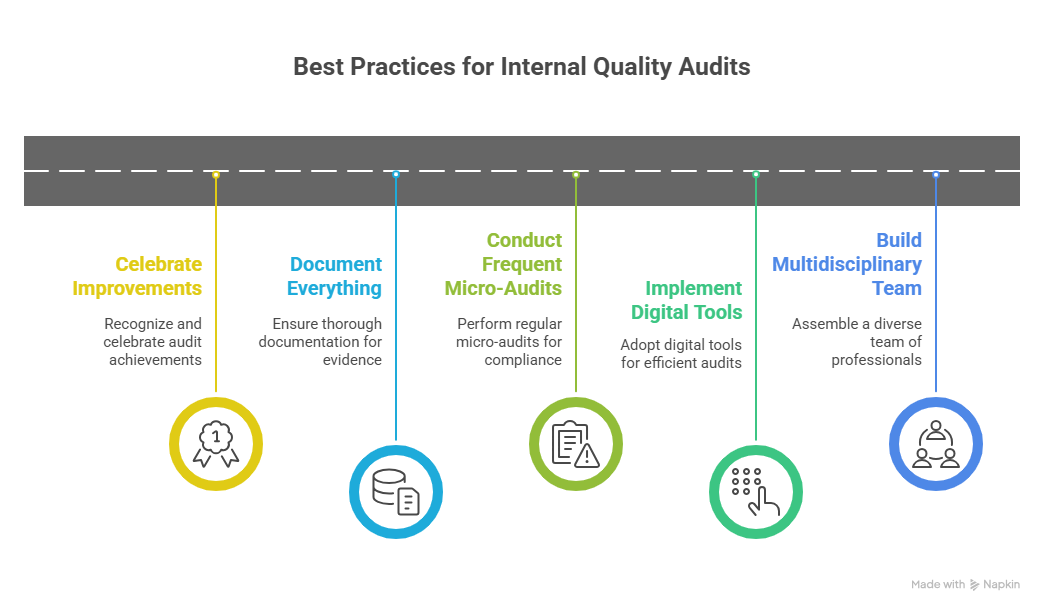
Below are proven strategies adopted by high-performing hospitals.
- Build a Multidisciplinary Audit Team
Include:
- Nurses
- Doctors
- Quality managers
- Biomedical engineers
- Pharmacists
- HR
- Facility management
Diverse teams identify more issues accurately.
- Implement Digital Audit Tools
Benefits include:
- Real-time evidence capture
- Automated reporting
- Trend analysis
- CAPA tracking
- Reduced paperwork
Digital tools speed up compliance and create transparency.
- Conduct Frequent Micro-Audits
Micro-audits help maintain daily compliance:
- Daily: hand hygiene
- Weekly: medication storage
- Monthly: facility safety
- Quarterly: documentation audits
- Document Everything — Evidence Matters
Assessors look for:
- Proof of implementation
- Proof of monitoring
- Proof of improvement
Internal audits ensure complete and reliable evidence.
- Celebrate Improvements
Recognition boosts motivation.
Celebrate:
- Zero nonconformities
- High compliance scores
- Best-performing departments
VIII. Conclusion: Internal Audits Are Your Strategic Advantage
Accreditation may seem overwhelming, but internal quality audits make it manageable, predictable, and achievable. They uncover risks early, strengthen compliance, improve safety, and build a culture of everyday readiness.
The most successful hospitals understand:
Accreditation isn’t won on the assessment day — it’s won in the months of disciplined internal auditing that come before it.
By investing in strong internal audit systems, your hospital can:
- Reduce accreditation risk
- Improve compliance consistency
- Enhance patient safety
- Boost staff confidence
- Strengthen governance
- Save significant time and cost
If you’re ready to elevate your hospital’s accreditation readiness, the first step begins with your internal audits.




